Manitoba's COVID Hospitals: A Tale of Two Realities – Optimism from the Top, Crisis Warnings from the Front Lines
Manitoba's healthcare system finds itself at a critical juncture, grappling with a significant surge in COVID-19 hospitalizations. As the province navigates this escalating challenge, a palpable tension exists between the reassurances offered by political leadership and the urgent warnings from medical professionals on the ground. While Manitoba's Health Minister expresses confidence in the system's capacity, doctors are sounding alarms, fearing an imminent crisis that could overwhelm hospitals and their dedicated staff.
The latest figures paint a concerning picture: a record 83 individuals hospitalized for COVID-19, with 15 requiring intensive care, as of recent reports. These numbers are not mere statistics; they represent a growing strain on resources, personnel, and infrastructure, pushing the provincial healthcare system closer to its limits.
The Minister's Perspective: Reassurance Amid Rising Numbers
Cameron Friesen, Manitoba's Health Minister, has consistently maintained that the province has not yet reached a breaking point in its ability to manage the pandemic within hospitals. Speaking to reporters, Friesen acknowledged the unwelcome upward trend in hospitalizations but emphasized the system's resilience and planning. "We are aware of the fact that there are more people hospitalized today than two weeks ago. Obviously, no one in Manitoba would want the numbers to go in that direction," he stated. Despite the increasing strain, the **Ministre de la Santé** (Health Minister) assured the public that the province retains various options to manage patient flow, indicating a prepared response to worsening scenarios.
Friesen's message aims to instill confidence, suggesting that while the situation is serious, the province is actively planning and adapting. He articulated a clear stance: "We are planning accordingly. We are not at a breaking point." This perspective highlights the government's commitment to maintaining a functional healthcare system even under duress, ensuring that critical care remains available to those who need it.
Doctors on the Front Lines: A Looming Crisis
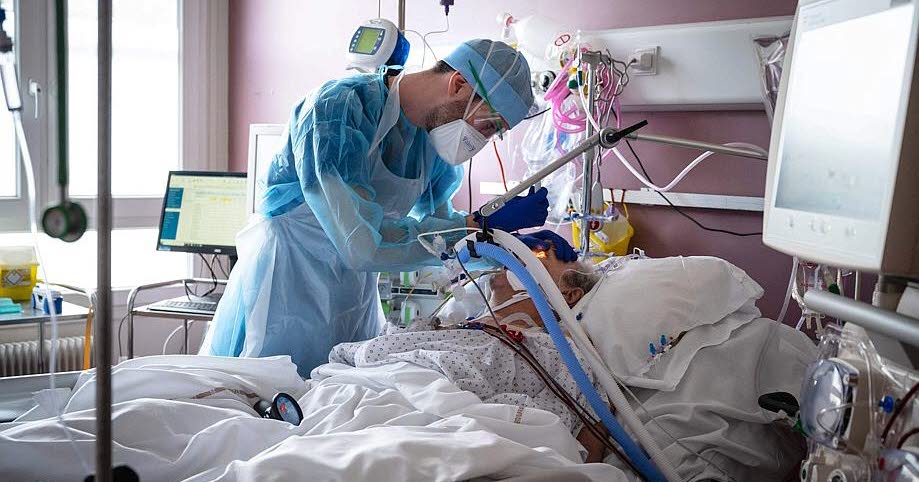
In stark contrast to the minister's optimism, healthcare professionals on the front lines are voicing grave concerns, painting a picture of a system teetering on the brink. Dr. Philippe Lagacé-Wiens, a medical microbiologist and physician at St. Boniface Hospital in Winnipeg, issued a stark warning that the city's intensive care units (ICUs) could reach maximum capacity within days. His dire prediction is not made lightly but stems from the daily realities faced by his colleagues and himself.
Dr. Lagacé-Wiens explicitly stated his worry that Manitoba could experience "horror stories similar to those that occurred in Europe in April and May." This reference to the devastating scenes witnessed internationally underscores the potential severity of the situation if the current trajectory continues unchecked. For a broader perspective on the gravity of such warnings, consider how other European officials have addressed similar crises, such as the
German Health Minister Issues Stark COVID Warning for Winter. The doctor's plea for recognition of the multifaceted nature of a healthcare crisis goes beyond simple bed counts, emphasizing the intricate web of resources required for effective patient care.
Beyond Bed Counts: The Multifaceted Strain on Healthcare
The concept of a healthcare system reaching its "code red" is far more complex than merely exhausting the number of available beds. As Dr. Lagacé-Wiens explained, the capacity of the system is determined by several critical factors:
- Number of Beds: While a primary concern, it's just one piece of the puzzle.
- Specialized Staff: The availability of highly trained nurses, doctors, and other medical personnel proficient in intensive care is paramount. These professionals cannot be easily replaced or trained overnight.
- Personal Protective Equipment (PPE): Adequate supplies of masks, gowns, and other protective gear are crucial not only for patient safety but also for protecting the healthcare workers themselves.
- Staffing Shortages Due to Isolation: A particularly insidious challenge is the increasing number of healthcare workers forced into isolation due to exposure to COVID-19 or active infections. This directly reduces the available workforce, creating a vicious cycle of strain.
This last point is especially alarming. Outbreaks have been reported at key facilities like St. Boniface Hospital and Victoria Hospital, leading to tragic outcomes including multiple deaths. When staff members at these hospitals contract the virus or are exposed, they must isolate, further depleting an already stretched workforce. This forces remaining staff to work longer hours, increasing stress and the risk of burnout. "What worries me is the remaining staff and the increased stress they will be under, because they will be asked for more and more hours," Dr. Lagacé-Wiens lamented. This growing pressure on healthcare workers can compromise their well-being and potentially impact the quality of care they can provide. The current challenges mirror broader trends, as explored in articles like
Manitoba Hospitals Face Record COVID Strain Amid Staff Shortages.
Proactive Measures and Public Responsibility
Manitoba's Health Minister, in his role as **Ministre Sante Covid** decision-maker, indicated that the province is preparing for various scenarios, including the potential cancellation of non-urgent surgeries. This measure, previously implemented during earlier waves of the pandemic, highlights the gravity of the situation and the difficult choices healthcare leaders face to preserve critical capacity. While necessary, deferring elective procedures has significant consequences for patients awaiting crucial treatments, underscoring the ripple effect of pandemic-related hospital strain.
The responsibility to alleviate pressure on the healthcare system does not solely rest with government officials and medical professionals. Public adherence to health guidelines is crucial. Practical tips for reducing community transmission and, consequently, hospitalizations include:
- Mask-Wearing: Consistent and proper use of masks in public settings significantly reduces viral spread.
- Physical Distancing: Maintaining a safe distance from others helps prevent close-contact transmission.
- Hand Hygiene: Frequent hand washing or sanitizing is a simple yet effective barrier against infection.
- Staying Home When Sick: Even mild symptoms warrant self-isolation and testing to prevent further spread.
- Getting Vaccinated (when eligible): Vaccination dramatically reduces the risk of severe illness, hospitalization, and death from COVID-19, easing the burden on hospitals.
These collective actions are vital. Every infection prevented means one less potential hospitalization, freeing up critical resources for other patients and reducing the immense stress on dedicated healthcare teams.
Conclusion: A United Front for Manitoba's Health
The contrasting perspectives of Manitoba's Health Minister and frontline doctors reflect the complex reality of managing a pandemic. While the province's **Ministre de la Santé** offers reassurance about existing plans and capacity, the medical community underscores the immediate and tangible risks of an overburdened system. With 83 people hospitalized and 15 in intensive care, and a total of 58 deaths recorded since the pandemic's outset in Manitoba, the numbers speak to a growing crisis. The ongoing outbreaks within hospitals and the subsequent strain on staff highlight the fragility of the healthcare system when pushed to its limits. Overcoming this challenge requires not only strategic planning from the government but also a collective effort from every Manitoban to mitigate the spread of the virus, support healthcare workers, and safeguard the province's vital health infrastructure. The path forward demands vigilance, empathy, and a shared commitment to public health.